Digital Health: Today’s Opportunity, Tomorrow’s Necessity
Examining digital health's current landscape, challenges, and opportunities to displace the current approaches in healthcare delivery and management.
Since the 2019 pandemic, patient engagement with digital health solutions such as telemedicine has increased exponentially due to the need for accelerated and remote care. Prior to the pandemic, the public’s interest to monitor their health analytics and use health and wellness apps shifted traditional healthcare approaches to include more real-time and historical data to monitor health. Other areas like AI-powered diagnostics and remote monitoring devices are showing great potential to yield better diagnostic and prognostic results. Additionally, healthcare companies are investing in integrating technology into their clinical and operational processes to improve patient outcomes, enable faster scaling at a sustainable cost, and build competitive advantage. Overall, placing technology in the center of health delivery and management provides healthcare practitioners and their patients the ability to communicate, exchange information/data, and monitor disease at a significantly faster rate than ever and promote better health outcomes.
The tech giants like Apple, Amazon, and Uber have made significant investments in this area by leveraging their expansive market presence and repurposing their core technologies. Others have entered the space through acquisition such as BestBuy’s $400M purchase of Current Health in October 2021.
With the giants stepping in, how can smaller firms compete and what does it take to win in this competitive yet fairly untapped market?
First, What is “Digital Health” Anyway?
Digital health refers to the integration of digital technologies, such as mobile devices, wearables, and software applications, into healthcare delivery and management. It involves the use of information and communication technologies (ICT) to improve healthcare services, promote wellness, and manage diseases. Digital health has the potential to increase access to healthcare, reduce costs, and improve the quality of care by providing patients with personalized and real-time health data. It encompasses a wide range of applications, from telemedicine and electronic health records to health and wellness apps, remote monitoring devices, and artificial intelligence-powered diagnostic tools.
Digital health encompasses a broad range of technologies and applications with a total market size of $185.5B and expect to grow rapidly.
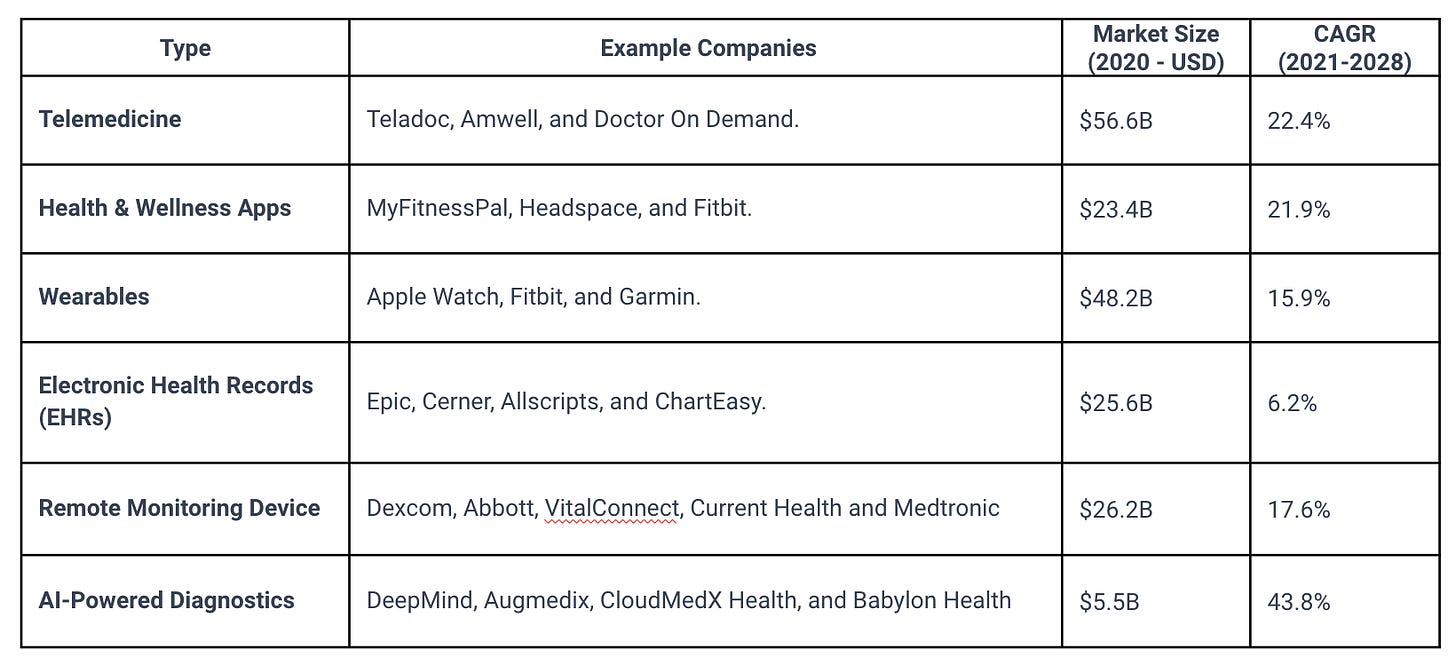
The current regulatory landscape of digital health and its future position
The regulatory landscape of digital health is rapidly evolving, and varies across different countries and regions. Here are some of the key regulatory frameworks that are currently in place:
United States: In the US, the Food and Drug Administration (FDA) is responsible for regulating medical devices, including digital health products. The FDA's regulatory approach to digital health is based on risk classification, with higher-risk products subject to more rigorous pre-market review and approval processes. The FDA has also established a Digital Health Center of Excellence to support the development and regulation of digital health products. Declaration of Public Health Emergency (PHE), authorized an expansive range of digital health solutions with great emphasis on telemedicine. According to McKinsey & Company, in 2019, only 11% of US consumers had used telemedicine. In April 2020, telemedicine adoption had increased by 50% compared to pre-pandemic levels. According to a survey by the American Medical Association, 28% of physicians reported using telemedicine for the first time during the pandemic. The United States is an obvious leader in this space with key announcements related to ending the PHE.
Reimbursement: Before the pandemic, Medicare had limited reimbursement for telemedicine services, but during the PHE, it expanded coverage and reimbursement rates. After the PHE, some of these changes may be extended, but it is uncertain whether all will be maintained. Commercial insurance plans may also have varying reimbursement policies for telemedicine services.
Licensure: During the PHE, many states temporarily waived or relaxed licensure requirements for out-of-state healthcare providers to practice telemedicine across state lines. As the PHE ends, some states may continue to allow this, but others may revert to previous licensure requirements.
Technology: During the PHE, healthcare providers were allowed to use a wider range of technologies to deliver telemedicine services, including phone calls and video conferencing platforms that were not previously approved. After the PHE, some of these relaxed policies may continue, while others may revert to previous regulations.
European Union: In the EU, digital health products are subject to regulation under the Medical Devices Regulation (MDR) and the In Vitro Diagnostic Regulation (IVDR). These regulations establish a framework for the classification, evaluation, and market authorization of medical devices, including digital health products.
Canada: Health Canada is responsible for regulating medical devices, including digital health products. The agency has established a framework for the classification and review of digital health products based on risk, and has launched initiatives to support the development of innovative digital health solutions.
Asia-Pacific: The regulatory landscape of digital health in the Asia-Pacific region varies across different countries. Some countries, such as Japan and South Korea, have established regulatory frameworks for digital health products, while others are still in the process of developing guidelines.
Foley & Lardner’s Healthcare Law Today summarized the new changes related to telemedicine, RPM, controlled substances, and reimbursement. Overall, the pandemic accelerated the growth of telemedicine and shifted attitudes towards the use of virtual care.
Barriers to patient and market adoption
While digital health has the potential to transform healthcare delivery and improve patient outcomes, there are several barriers to its widespread adoption that need to be addressed to scale:
Privacy and security concerns: The use of digital technologies to collect and store health data raises concerns about the privacy and security of that data. Patients may be hesitant to use digital health tools if they are unsure that their data is being protected.
Lack of interoperability: Different digital health tools may not be able to communicate with each other, which can make it difficult for healthcare providers to access a complete picture of a patient's health. This lack of interoperability can also make it difficult to share health data between providers.
Cost and reimbursement: Digital health tools may be expensive to develop and implement, and there may be limited reimbursement for these services. This can make it difficult for healthcare providers to invest in digital health technologies.
Limited access to technology: Not all patients have access to the technology needed to use digital health tools, such as smartphones or high-speed internet. This can create disparities in healthcare access and outcomes.
Resistance to change: Some healthcare providers may be resistant to adopting new technologies or changing established workflows. This can make it difficult to implement digital health tools effectively.
Addressing these barriers will be critical to realizing the full potential of digital health and improving healthcare outcomes for all patients.
How can the little guys compete with the big boys of the industry?
The tech giants are applying their expansive reach and adapting their existing technology to compete in the digital health space. This means that the smaller players must quickly find their competitive edge, build a strong customer base, and scale to sustain and grow a strong position against the giants.
Products and in turn companies win that can solve a pervasive problem and/or create new ecosystems that satisfy an unanticipated unmet need. The digital health industry players will win if they are able to create affordable, accessible, and useful solutions to create value for their users while defending their competitive advantage over time. Companies like Biofourmis and BetterHelp leverage unique technologies such as AI/ML and/or an easy to navigate platform to create value. At their core, the winners leverage Human-Centered Design to build seamless applications and ecosystems tailored to human intuition and muscle memory.
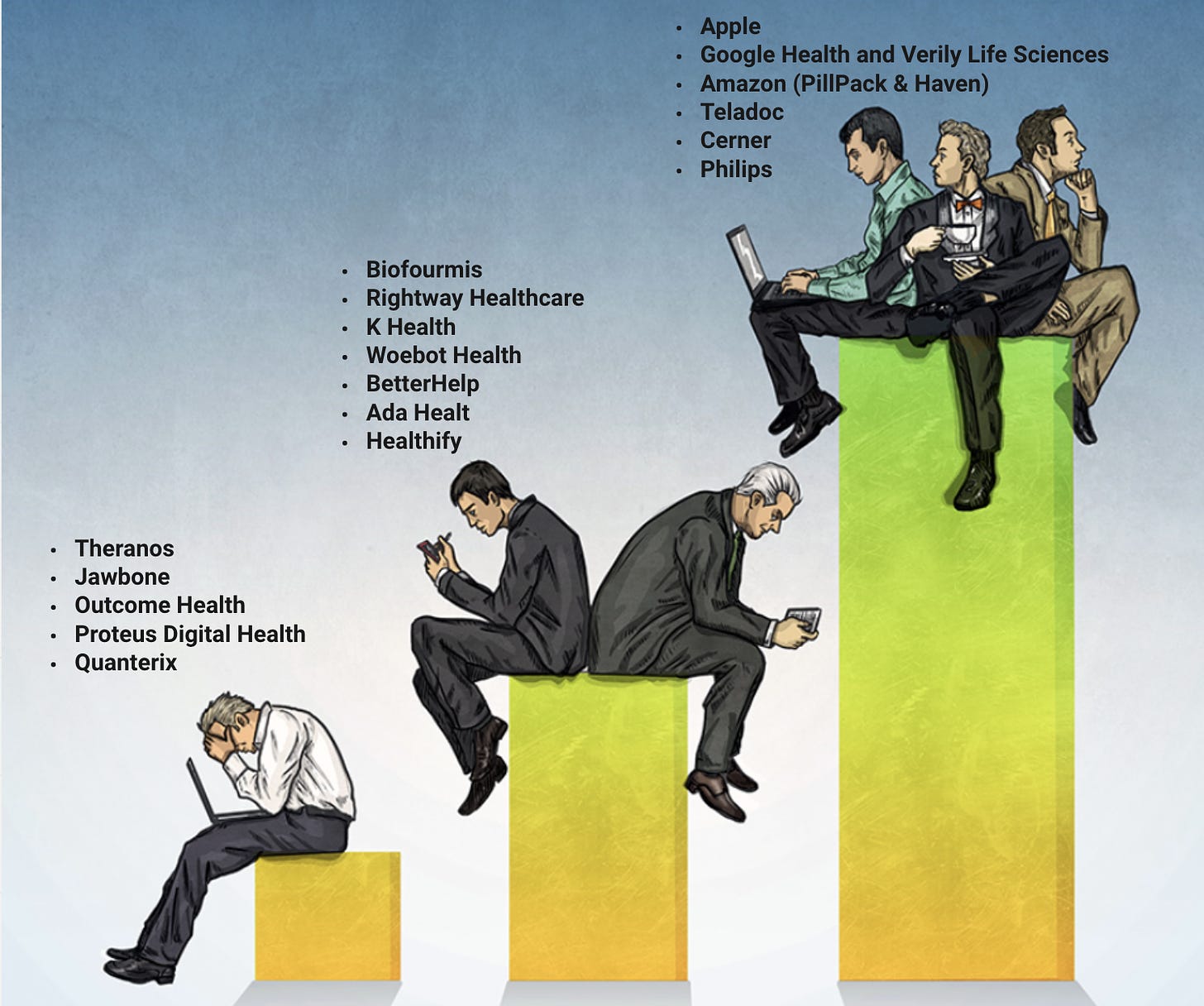
Here’s a short list of some of the giants, some breakout winners and a hefty list of losers to name a few.
So, what’s the secret to winning in this space? Some to consider incorporating into your products would be as follows:
Incorporating Human-centered design
Responsible use of gamification and captology in design
Digital transformation
Strategic resource deployment
Adjacent market development
People and process management
Increasing digital health adoption by incorporating human-centered design into development
Human-centered design (HCD) is a design approach that puts the needs, preferences, and experiences of users at the center of the design process. In the context of digital health, HCD involves designing digital health tools and technologies that are user-friendly, accessible, and tailored to the needs of patients and healthcare providers. HCD in digital health can lead to more effective and efficient healthcare delivery, improved patient outcomes, and increased patient engagement. It can also help address some of the barriers to digital health adoption, such as privacy and security concerns, limited access to technology, and resistance to change. By involving patients and healthcare providers in the design process and continuously gathering feedback, HCD can ensure that digital health solutions are user-centered and meet the unique needs of different patient populations. Overall, HCD is a critical component of successful digital health initiatives that prioritize patient-centric care.
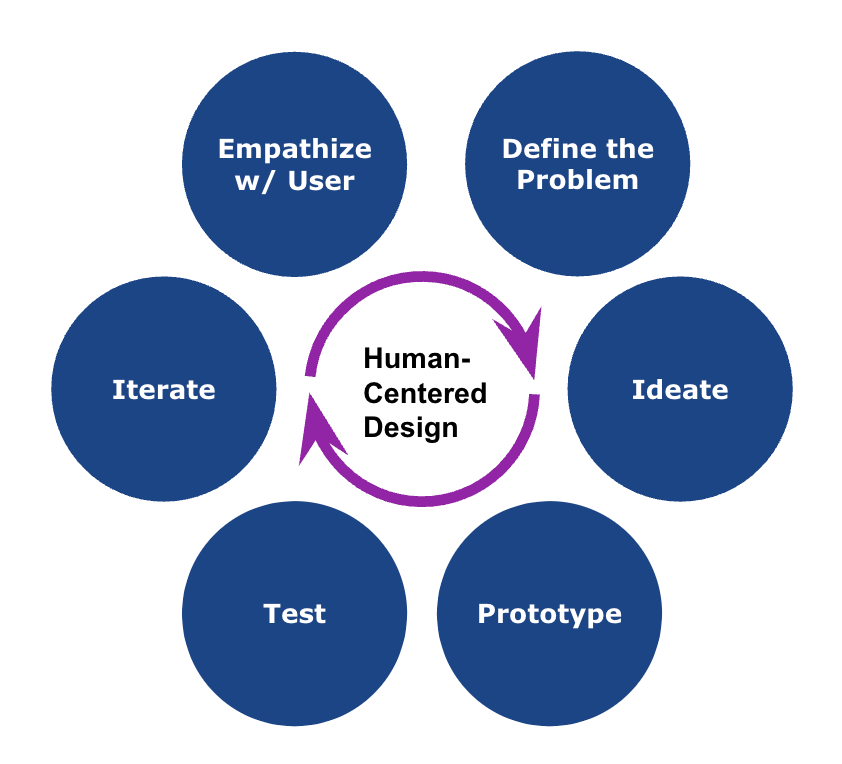
HCD involve a series of iterative steps to understand the users’ need, build and test prototypes that address their pain points and continue to improve over time (Figure-1).
Influencing human behavior - responsibly!
In the last decade, applications that influence human behavior have received a lot of backlash, and for good reason. These apps such as Facebook, Instagram, Twitter, and others make use of captology and gamification to influence and engage users. While we have seen a negative and at times irresponsible use of these approaches, their responsible use can be powerful to improving human health.
Captology, also known as persuasive technology, is a field of study that examines the design, development, and use of interactive computing systems that are intended to change people's attitudes or behaviors. The term "captology" was coined by psychologist and researcher B.J. Fogg, who founded the Persuasive Technology Lab at Stanford University in the 1990s.
Captology involves the use of technology to influence human behavior in various ways, such as promoting healthy habits, improving learning outcomes, and increasing productivity. Some examples of captology in action include fitness apps that encourage users to exercise regularly, educational games that help students learn new concepts, and productivity tools that motivate users to complete tasks on time.
While captology has the potential to bring about positive changes in people's lives, it also raises ethical and privacy concerns. Critics argue that persuasive technology can be used to manipulate people's behavior without their consent, and that it may infringe on individual autonomy and freedom of choice. As such, researchers and designers in the field of captology are encouraged to consider the potential risks and benefits of their work, and to prioritize user consent and privacy in their designs.
On the other hand, gamification refers to the process of applying game mechanics and design elements to non-game contexts, such as education, marketing, or healthcare, to engage users and motivate them to achieve certain goals. Gamification involves creating a game-like experience that encourages users to take specific actions or complete certain tasks, often by using rewards, points, badges, leaderboards, or other similar techniques. The main goal of gamification is to increase user engagement, motivation, and participation by making the experience more enjoyable and rewarding.
While both gamification and captology involve using design elements to influence human behavior, the key difference is that gamification uses game mechanics specifically to engage users, while captology can use a variety of design elements to persuade people to take a certain action or adopt a specific attitude or belief. In other words, gamification is a specific type of captology that uses game-like elements to motivate and engage users.
Run, don’t walk!! Why everyone should learn about digital transformation?
Digital transformation is a rather broad term; however, its application in healthcare involves the use of technology to improve the quality, efficiency, and accessibility of healthcare services and position the service providers to replace old and existing internal workflows with technology and automation. Non-integrated systems present another challenge not only in care delivery but in management of operations and ensuring compliance.
Companies are dedicating significant resources to transforming their old and outdated systems with newer and more capable alternatives putting integration and interoperability at the top of their planning. Building a streamlined workflow starts with evaluating the current technology stack with the desired results in mind to stitch together the best and most cost-effective set of systems and applications to accomplish the intended goals for the organization. This process also includes setting a “build vs. buy” strategy and performing a comprehensive analysis of the technology suites and options that work best together. To compete with the tech giants and smart players in the field, companies must set digital transformation at the top of their 3-5 year strategic planning to succeed.
Where to point that laser?
Deliberate and effective allocation of resources is essential to maximizing margins, gaining competitive advantage, improve productivity, and driving growth. These resources can include financial capital, human capital, technology, equipment, and more. Proper resource deployment requires careful planning and evaluation of a company's strengths, weaknesses, opportunities, and threats also knowns as SWOT analysis. By identifying areas where resources are most needed, businesses can optimize their operations, minimize waste, and maximize their chances of success. It is a critical aspect of strategic management, and companies that prioritize it tend to be more successful in the long run. It is very tempting to try to do everything and on the surface level it might even seem like it’s working; however, securing the company’s position in the market should be the first goal and until that is achieved, it is foolish to think that one can juggle and ride a bike when neither is perfected!
Venturing out to conquer new heights
Developing adjacent markets allows companies to leverage their existing capabilities, resources, and customer base to capture new revenue streams and gain a competitive advantage. For example, a company that produces fitness equipment may expand into the health and wellness industry by offering nutritional supplements or workout programs. Developing adjacent markets requires careful market research and analysis to identify opportunities that align with the company's core competencies and existing customer base. By expanding into adjacent markets, companies can diversify their revenue streams, reduce risk, and increase their overall market share. However, it is important for companies to approach adjacent market development with a clear understanding of their capabilities, competitive landscape, and potential risks.
Building a vault of knowledge in your people and process
The famous “product, people, process” may seem like a cliché; however, companies that build lasting competitive products always have good people and process. The pandemic necessitated lots of throwing things together to make things work both in hiring and building process but as we step out of the fog, it’s important to get back to the basics.
With that said, automating processes and freeing people to do the thinking, strategizing, and caring for patients should be the guiding principle to stay competitive long term.
As always, would love to hear from you. Feel free to email me, reach out on LinkedIn, or comment here.